Content
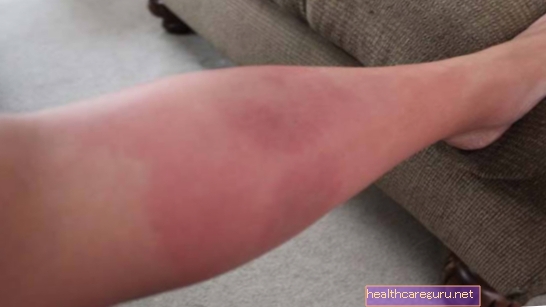
Infectious cellulitis, also known as bacterial cellulitis, occurs when bacteria manage to enter the skin, infecting the deepest layers and causing symptoms such as intense redness of the skin, pain and swelling, especially in the lower limbs.
In contrast to the popular cellulite, which in reality is called fibro-edema geloid, infectious cellulitis can cause serious complications such as septicemia, which is the general infection of the organism, or even death, if not properly treated.
Thus, whenever a skin infection is suspected, it is very important to go to the emergency room to make the diagnosis and start the appropriate treatment, which is usually done with the use of antibiotics. See how the treatment is done.
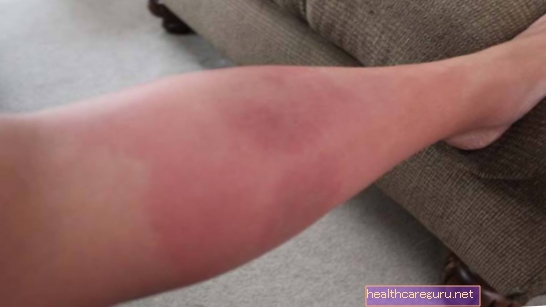
Main symptoms
Some of the symptoms that help to identify a case of infectious cellulitis include:
- Pain in the affected area;
- Extensive red regions across the body;
- Extensive and red region in the affected body part;
- Fever above 38ºC;
- Swelling of the skin, which may produce pus;
- Languages near the affected site.
In more severe cases, symptoms can also include tremors, chills, fatigue, dizziness, excessive sweating and muscle pain. Symptoms such as drowsiness, blisters or red rays on the skin may be signs that infectious cellulitis is getting worse.
All of these symptoms can also be a sign of other types of skin infection, especially erysipelas, which is a disease that affects the most superficial layers of the skin. Thus, one should consult a general practitioner or dermatologist to find out the correct cause, in order to start the most appropriate treatment.
How to confirm the diagnosis
In most cases, infectious cellulitis is identified by the dermatologist only by observing the signs and symptoms, however, as the symptoms can be very similar to other types of skin infection, especially erysipelas, the doctor may also order a skin exam. blood or even a laboratory test to evaluate a sample of the affected skin to confirm the type of bacteria causing the infection.
How to differentiate cellulite from erysipelas
The main difference between infectious cellulitis and erysipelas is that, while infectious cellulitis reaches deeper layers of the skin, in the case of erysipelas, the infection happens more on the surface. Still, some differences that can help to identify the two situations are:
| Erysipelas | Infectious Cellulite |
|---|
| Superficial infection | Infection of the deep dermis and subcutaneous tissue |
| It is easy to identify infected and uninfected tissue due to large stains | It is difficult to identify infected and uninfected tissue, with small spots |
| More frequent in the lower limbs and face | More frequent in the lower limbs |
However, the signs and symptoms of these diseases are very similar, so the general practitioner or dermatologist should examine the affected area and may order several tests to identify the correct cause, identify signs of severity and initiate the most effective treatment. Better understand what it is and how to treat erysipelas.
What can cause cellulite
Infectious cellulitis arises when bacteria of the type Staphylococcus or Streptococcus can penetrate the skin. Therefore, this type of infection is more common in people with surgical wounds or cuts and stings that have not been properly treated.
In addition, people with skin problems that can cause skin discontinuity, as in eczema, dermatitis or ringworm, are also at higher risk of developing a case of infectious cellulitis, as well as people with weakened immune systems, for example.
Is infectious cellulitis contagious?
In healthy people, infectious cellulite is not contagious, as it does not catch easily from one person to another. However, if someone has a skin wound or disease, such as dermatitis, for example, and comes into direct contact with the area affected by cellulite, there is a higher risk that the bacteria will penetrate the skin and cause infectious cellulitis.
How the treatment is done
Treatment for infectious cellulitis is usually started with the use of oral antibiotics, such as Clindamycin or Cephalexin, for 10 to 21 days. During this period it is advisable to take all tablets at the time indicated by the doctor, as well as to observe the evolution of redness on the skin. If the redness increases, or another symptom gets worse, it is very important to go back to the doctor, as the antibiotic prescribed may not be having the expected effect and needs to be changed.
In addition, the doctor may also prescribe pain relievers, such as Paracetamol or Dipyrone, to relieve symptoms during treatment. It is also important to examine the skin regularly, make a wound dressing at the health center, or even apply a suitable cream containing antibiotics, which can be recommended by the doctor to ensure the success of the treatment.
Normally, symptoms improve within 10 days of starting antibiotics, but if symptoms worsen it may be necessary to change antibiotics or even stay in the hospital to do the treatment directly in the vein and prevent the infection from spreading through the body.
Better understand how the treatment is done and what the signs of improvement are.