Content
Scleroderma is a chronic autoimmune disease in which there is excessive production of collagen, leading to hardening of the skin and affecting the joints, muscles, blood vessels and some internal organs, such as the lungs and heart.
This disease mainly affects women over 30, but it can also occur in men and children, and is divided into two types, localized and systemic scleroderma, according to its intensity. Scleroderma has no cure and its treatment is done to relieve symptoms and slow the progression of the disease.
Scleroderma symptoms
Scleroderma symptoms evolve over time and, according to the location of the symptoms, scleroderma can be classified into:
- Systemic, in which symptoms are manifested in the skin and internal organs, being considered the most severe form of scleroderma;
- Located, where symptoms are restricted to the skin.
In general, the main symptoms related to scleroderma are:
- Thickening and stiffness of the skin;
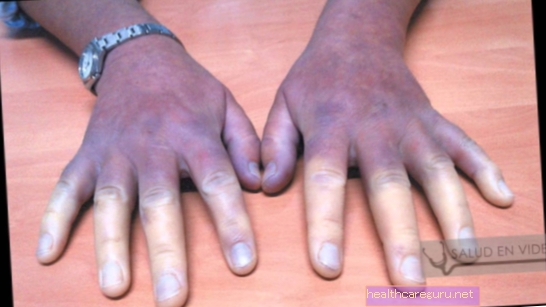
- Constant swelling of fingers and hands;
- Darkening of the fingers in cold places or during episodes of excessive stress, also known as Raynaud's phenomenon;
- Constant itching in the affected region;
- Loss of hair;
- Very dark and very light spots on the skin;
- Appearance of red spots on the face.
The first manifestations of the disease start on the hands and after months or years pass to the face, leaving the skin hardened, without elasticity and without wrinkles, which also makes it difficult to open the mouth completely. In addition, in cases of systemic scleroderma, the person may also have increased blood pressure, poor digestion, shortness of breath, weight loss without an apparent cause, changes in the liver and heart.
Possible complications
Complications of scleroderma are related to the beginning of treatment and are more frequent in people who have the systemic form of the disease. Thus, when the treatment is not done according to the doctor's guidance, the person develops some complications such as difficulty in moving the fingers, swallowing or breathing, anemia, arthritis, heart problems and kidney failure, for example.
How the diagnosis is made
The diagnosis of scleroderma is difficult, as the symptoms progress slowly and can be confused with other skin problems. The disease must be confirmed by the dermatologist or rheumatologist, taking into account the signs and symptoms presented by the person, and the result of imaging and laboratory tests.
Thus, a CT scan or chest X-ray and skin biopsy may be indicated by the doctor, in addition to the ANA test, which is a laboratory test that aims to identify the presence of self- antibodies circulating in the blood.
Treatment of scleroderma
Scleroderma has no cure and, therefore, treatment aims to prevent disease progression, relieve symptoms and promote the person's quality of life. The treatment indicated by the rheumatologist or dermatologist may vary according to the type of scleroderma and symptoms presented by the person, and the use of some remedies may be indicated according to the case, which can be applied directly to the skin or ingested, such as immunosuppressants or corticosteroids. .
In the case of people who present Raynaud's phenomenon as one of the scleroderma symptoms, it is also indicated that they keep the extremities of the body warm.
In addition, as scleroderma may be related to joint stiffness, physiotherapy sessions may also be indicated to increase joint flexibility, decrease pain, prevent contractures and maintain limb function and amplitude.