Content
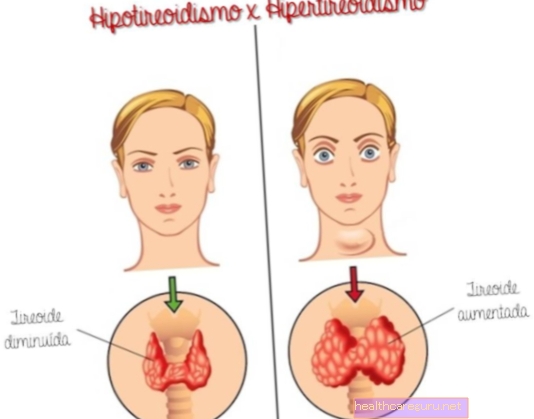
Hypothyroidism in pregnancy when unidentified and treated can cause complications for the baby, because the baby needs the thyroid hormones produced by the mother to be able to develop correctly. Therefore, when there is little or no amount of thyroid hormones, such as T3 and T4, there can be miscarriage, delayed mental development and decreased intelligence quotient, the IQ.
In addition, hypothyroidism can decrease the chances of becoming pregnant because it alters a woman's reproductive hormones, causing ovulation and the fertile period not to occur during the menstrual cycle. Therefore, it is important that pregnant women are monitored by the obstetrician and TSH, T3 and T4 measurements are performed to identify hypothyroidism and treatment is started if necessary.
Risks for mother and baby
Hypothyroidism in pregnancy can cause complications for both mother and baby, especially when the diagnosis is not made and when the treatment is not started or performed correctly. The baby's development is completely dependent, especially in the first 12 weeks of pregnancy, on thyroid hormones produced by the mother. Thus, when the woman has hypothyroidism, there is an increased risk of consequences and complications for the baby, the main ones being:
- Cardiac changes;
- Delayed mental development;
- Decreased intelligence quotient, IQ;
- Fetal distress, which is a rare condition characterized by decreased oxygen supply to the baby, interfering with the baby's growth and development;
- Low weight at birth;
- Speech alteration.
In addition to having risks for the baby, women with unidentified or treated hypothyroidism are at increased risk of developing anemia, placenta previa, bleeding after childbirth, premature birth and having pre-eclampsia, which is a condition that tends to start from 20 weeks of gestation and causes high blood pressure in the mother, which can affect the proper functioning of the organs and cause miscarriage or premature birth. See more about pre-eclampsia and how to treat it.
Can hypothyroidism make pregnancy difficult?
Hypothyroidism can make pregnancy difficult because it can change the menstrual cycle and influence ovulation, and in some cases there may not be an egg release. This is because thyroid hormones have an influence on the production of female sex hormones, which are responsible for the menstrual cycle and the woman's fertility.
So, to get pregnant even if you have hypothyroidism, you must keep the disease well controlled, doing blood tests to assess hormone levels and correctly doing the treatment recommended by the doctor.
When controlling the disease, the hormones of the reproductive system are also more controlled and, after about 3 months it is possible to become pregnant normally.However, it is necessary to continue doing blood tests regularly, to assess the need to adjust medications and respective doses.
In addition, in order for pregnancy to be possible, it is important that the woman check whether her menstrual cycle has managed to become more or less regular and, with the help of the gynecologist, identify the fertile period, which corresponds to the period in which there is a greater probability of pregnancy. pregnancy. Find out when the fertile period is by taking the following test:
How to identify
In most cases, pregnant women already have hypothyroidism before pregnancy, but prenatal tests help to detect diseases in women who did not have symptoms of the problem.
In order to diagnose the disease, blood tests should be carried out to assess the amount of thyroid hormones in the body, with TSH, T3, T4 and thyroid antibodies and, in positive cases, repeat the analysis every 4 or 8 weeks. throughout pregnancy to maintain control of the disease.
How treatment should be
If the woman already has hypothyroidism and plans to become pregnant, she must keep the disease well controlled and have blood tests every 6 to 8 weeks since the first trimester of pregnancy, and the dose of the medication should be higher than before pregnancy, and follow the recommendations of the obstetrician or endocrinologist.
When the disease is discovered during pregnancy, the use of drugs to replace thyroid hormones should begin as soon as the problem is identified, and the analyzes should also be repeated every 6 or 8 weeks to readjust the dose.
Hypothyroidism in the postpartum
In addition to the gestation period, hypothyroidism can also appear in the first year after delivery, especially 3 or 4 months after the baby is born. This is due to changes in the woman's immune system, which proceeds to destroy thyroid cells. In most cases, the problem is temporary and resolves within 1 year of postpartum, but some women develop permanent hypothyroidism, and all are more likely to have the problem again in a future pregnancy.
Thus, one must be attentive to the symptoms of the disease and have blood tests that assess the functioning of the thyroid during the first year after delivery. So, see what the symptoms of hypothyroidism are.
Watch the following video to learn what to eat to prevent thyroid problems: