Content
Malaria is an infectious disease transmitted through the bite of the female mosquito Anopheles infected by the protozoan of the genus Plasmodium, being the most frequent species in Brazil the Plasmodium vivax it's the Plasmodium malariae. Because it is transmitted by the bite of a mosquito, the best way to prevent malaria consists of measures to prevent getting bitten, through the use of repellent and window protection with the use of screens.
Once in the affected person's body, the Plasmodium it goes to the liver, where it multiplies and then reaches the bloodstream, where it invades and breaks the red blood cells, causing symptoms such as fever, sweat, chills, nausea, vomiting, headache and weakness.
Malaria is curable, but it is important that treatment is started quickly, as in many cases the disease can become severe, with anemia, decreased platelets, kidney failure or even impairment of the brain, in which the chances of complications and death are greater.
Malaria mosquito
Main symptoms
The first symptoms of malaria usually appear between 8 to 14 days after transmission, and can take up to 30 days or more. The appearance of symptoms depends on factors related to the Plasmodium, such as multiplication rate and species, and factors related to the person, such as the immune system, mainly. The most common signs and symptoms of malaria are:
- Fever, which can come and go in cycles;
- Sweats and chills;
- Strong headache;
- Nausea and vomiting;
- Muscle pain throughout the body;
- Weakness and constant tiredness;
- Yellowed skin and eye.
Most of these signs and symptoms can be difficult to identify as malaria, so if they do occur, it is important to go to the doctor to diagnose the disease and start appropriate treatment, especially if you are in a place where malaria is common, as in Amazon region and Africa.
In addition, these signs and symptoms may appear in cycles, that is, they appear every 48 hours or 72 hours, depending on the species Plasmodium that is infecting the body. This happens due to their life cycle, as they develop they reach the bloodstream and cause symptoms resulting from the destruction of red blood cells.
The most severe form of malaria occurs when the infection affects the brain, causing headache, neck stiffness, seizures, drowsiness and coma. Other complications include anemia, reduced platelets, kidney failure and respiratory failure. Learn more about the symptoms of malaria and cerebral malaria.
How the transmission happens
Malaria transmission occurs through the bite of the female mosquito Anopheles infected, which acquired the parasite when biting a person infected by the disease. It is important to remember that malaria is not contagious, that is, it is not transmitted from one person to another, except in the rarest cases of sharing infected syringes and needles, poorly controlled transfusions and / or delivery.
Usually, the mosquito bites people at dusk or dusk. The places with the highest risk of contamination are South America, Central America, Africa and part of Asia, mainly in places with clean water with little current, humidity and temperatures between 20º and 30ºC. In Brazil, the states most affected by malaria are Amazonas, Roraima, Acre, Tocantins, Pará, Amapá, Mato Grosso, Maranhão and Rondônia.
Malaria infection cycle
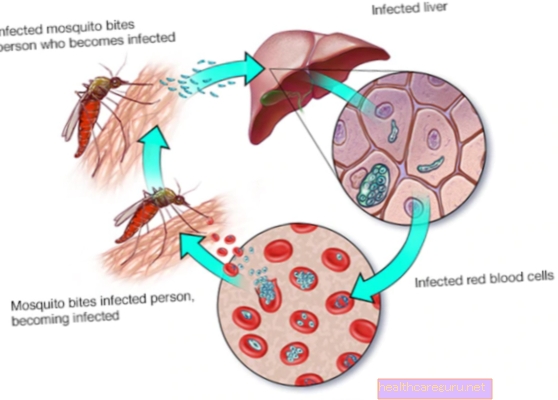
The parasite cycle Plasmodium in the human body happens as follows:
- The bite of the female mosquito Anopheles transmits, through its saliva, the Plasmodium to the person's bloodstream, in its Sporozoite phase;
- Sporozoites go to the liver, where they mature and multiply, for about 15 days, giving rise to the form of Merozoites;
- Merozoites disrupt liver cells and reach the bloodstream, starting to invade red blood cells;
- Within the infected blood cells, which are called Schizonts, the parasites multiply and disrupt this cell, and begin to invade others, in a cycle that lasts 48 to 72 hours.
Within each schizont, the cycle is variable according to the species of the Plasmodium, being 48 hours for species P. falciparum, P. vivax, and P. ovale and 72 h for P. malariae. During the period when the red blood cells are ruptured and the schizonts become free in the blood, the symptoms can become more pronounced, mainly fever and chills.
How to confirm the diagnosis
After the first signs and symptoms appear, it is recommended to go to the hospital or emergency room, especially if the symptoms appear every 48 or 72 hours. In this way, the doctor will be able to identify the presence of the parasite in the body through blood tests, as he likes thick or immunological tests, being able to start the appropriate treatment, preventing the infection from aggravating and putting the patient's life at risk.
How the treatment is done
Malaria is treated with antimalarial drugs, such as Chloroquine, Primaquine, Artemeter and Lumefantrine or Artesunate and Mefloquine for example, which work by destroying the Plasmodium and preventing its transmission.
The chosen medications, doses and duration are indicated by the doctor according to age, severity of the disease and analysis of health conditions. Children, babies and pregnant women need special treatment, with Quinine or Clindamycin, always in accordance with medical recommendations and hospitalization is usually indicated.
It is also recommended:
- Eat normally;
- Do not consume alcoholic beverages;
- Do not stop the treatment even if the symptoms disappear, due to the risk of recurrence and complications of the disease.
Malaria treatment should be started as soon as possible, as it can progress severely and, without proper treatment, can lead to death. Learn more about how treatment is done to recover faster.
How to protect yourself
Malaria prevention can be done through:
- Use of light colored clothes and fine fabric, with long sleeves and long pants;
- Avoid the areas most prone to contamination of the disease, especially during dusk or dawn;
- Use DEET-based repellent (N-N-diethylmetatoluamide), respecting the manufacturer's guidelines for repellent replacement;
- Place mosquito protection screens on windows and doors;
- Avoid lakes, ponds and rivers in the late afternoon and evening.
Whoever travels to a place where there are cases of malaria can receive a preventive treatment, called chemoprophylaxis, with anti-malarial drugs, such as Doxycycline, Mefloquine or Chloroquine.
However, these drugs have strong side effects, so the doctor usually recommends this type of prevention for people who are at greater risk of developing serious illness, such as going to places with high rates of transmission or when the person has a disease that may have major complications. with the infection.
These drugs should only be used after medical advice and are usually started 1 day before travel and persist for a few more days or weeks after return.