Content
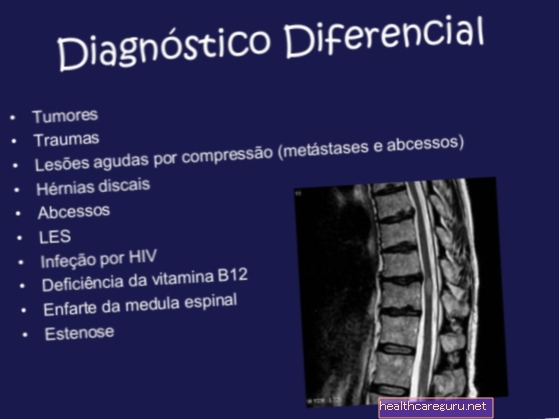
Transverse myelitis, or just myelitis, is an inflammation of the spinal cord that can occur as a result of infection by viruses or bacteria or as a result of autoimmune diseases, and which leads to the appearance of neurological signs and symptoms, with impairment of motor or sensitive, for example.
Thus, the main signs and symptoms of transverse myelitis happen due to bone marrow involvement, which can result in muscle paralysis in addition to back pain, muscle weakness, with decreased sensitivity and paralysis of the legs and / or arms.
Myelitis treatment aims to promote the person's quality of life and, therefore, the neurologist may recommend specific treatment for the cause of myelitis, and the treatment can be complemented by physiotherapy sessions, as this is possible stimulate muscle movement and prevent paralysis.
Symptoms of transverse myelitis
The symptoms of transverse myelitis arise due to the involvement of the peripheral nerves of the spine, and there may be:
- Spine pain, especially in the lower back;
- Tingling or burning sensation in the chest, abdomen, legs or arms;
- Weakness in arms or legs, with difficulty holding objects or walking;
- Tilt of the head forward, and difficulty swallowing;
- Difficulty holding urine or feces.
Since myelitis can affect the myelin sheath of nerve cells, the transmission of nerve stimuli is more impaired over time and, therefore, it is common for symptoms to get worse every day, becoming more intense, there may even be paralysis, which prevents the person from walking.
When the portion of the spine affects is lower, it is possible for the person to lose leg movements, and when the affected area is close to the neck, the affected person may lose shoulder and arm movements. In the most severe cases, it may be difficult to breathe and swallow, requiring hospitalization.
Thus, whenever symptoms appear that may indicate a problem in the spine, it is very important to consult a general practitioner or neurologist, for example, to identify the cause and start treatment, before lesions that are difficult to resolve appear. In this situation, after diagnosis it is normal for the person to be referred to a neurologist.
How to confirm the diagnosis
To make the diagnosis of myelitis, you should consult a general practitioner or a neurologist, when there is a lot of suspicion of a spinal problem. The doctor, in addition to assessing symptoms and a history of illness, usually also orders some diagnostic tests, such as MRI, lumbar puncture and various blood tests, which help to make the differential diagnosis and confirm the diagnosis of transverse myelitis.
Main causes
Transverse myelitis is a rare condition that can happen as a consequence of some situations, the main ones being:
- Viral infections, especially in the lung (Mycoplasma pneumoniae) or in the digestive system;
- Enteroviruses, such as EV-A71 and EV-D68;
- Rhinovirus;
- Infections by parasites, such as toxoplasmosis or cysticercosis;
- Multiple sclerosis;
- Optic neuromyelitis;
- Autoimmune diseases, such as lupus or Sjogren's syndrome.
Although it is very rare, there are also reports of cases of transverse myelitis that arose after taking a vaccine against hepatitis B or against measles, mumps and chicken pox. In addition, there is also a report that the symptoms of transverse myelitis developed in a person who received the experimental vaccine against the new coronavirus, SARS-CoV-2 / COVID-19, however this relationship is still being studied, as well as vaccine effectiveness.
How the treatment is done
The treatment of myelitis varies a lot according to each case, but it is usually started with the use of medicines to treat possible infections, reduce the inflammation of the spinal cord and relieve the symptoms, improving the quality of life. Some of the most commonly used medications include:
- Injectable corticosteroids, such as Methylprednisolone or Dexamethasone: quickly reduce inflammation of the spinal cord and decrease the response of the immune system, relieving symptoms;
- Plasma exchange therapy: it is used in people who have not improved with the injection of corticosteroids and works by removing excess antibodies that may be causing the inflammation of the spinal cord;
- Antiviral remedies: to treat any possible viral infection that is active and harming the spinal cord;
- Analgesics, such as acetaminophen or naproxen: to relieve muscle pain and any other type of pain that may arise.
After this initial therapy, and when symptoms are more controlled, the doctor may advise physiotherapy sessions to help strengthen the muscles and train coordination, which may be affected by the disease. Although physical therapy cannot cure the disease, it can greatly improve muscle strength, coordination of movements, facilitating own hygiene and other day-to-day tasks.
In some cases, occupational therapy sessions may still be necessary, so that the person learns to do daily activities with the new limitations that may arise with the disease. But in many cases there is a full recovery in a few weeks or months.